Protection Mode vs Creation Mode: The Missing Conversation in IVF Preparation
For years, IVF preparation has been framed as a checklist.
The right supplements.
The optimal hormone levels.
The perfect protocol.
We prepare the body carefully.
But we rarely prepare the environment the body is operating in — the nervous system.
And that environment matters more than most women realise.
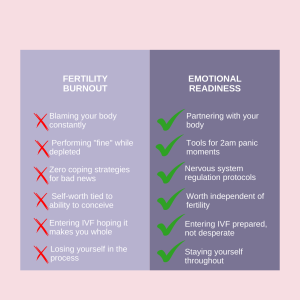
When we enter the IVF tunnel, many of us shift into what I call Protection Mode.
We become investigators of our own bodies.
Tracking.
Monitoring.
Scanning for signs.
It feels responsible.
But prolonged vigilance has a cost.
What Psychological Safety Actually Means
In fertility care, psychological safety is not about “staying positive.”
It is the felt sense that your body is not under threat.
It is the difference between your system feeling urgent and braced,
and feeling steady and regulated.
When your nervous system perceives safety, stress chemistry reduces and the body has greater capacity for repair and regulation.
Safety does not guarantee pregnancy.
But it changes the internal conditions in which conception is attempting to occur.
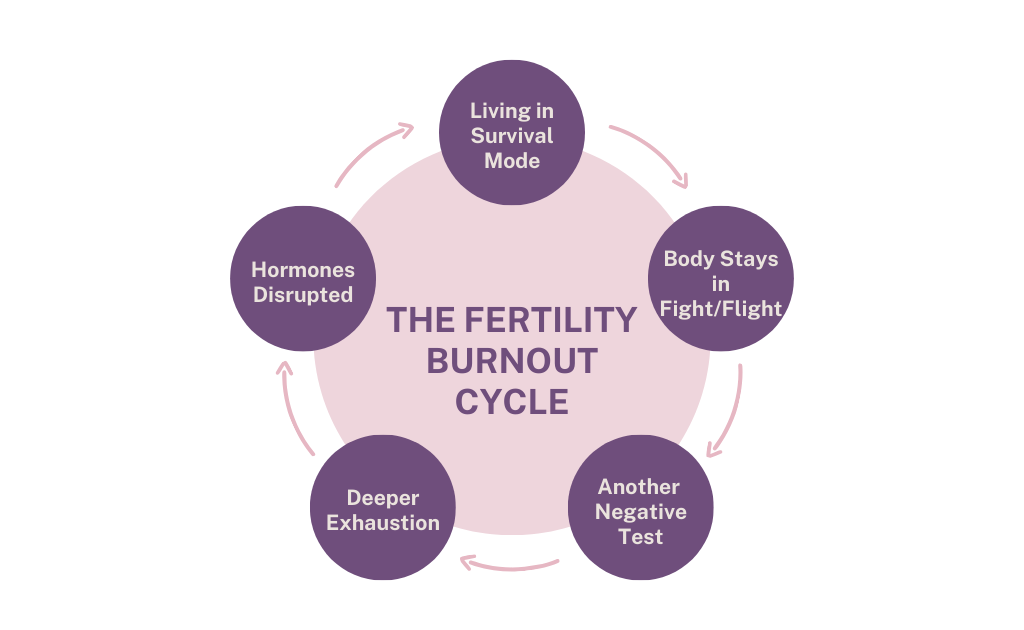
The Toll of Long-Haul IVF
Long-haul IVF often creates chronic vigilance.
You track LH peaks.
You analyse progesterone levels.
You read statistics late at night.
Over time, constant monitoring can keep the stress response activated.
When the brain repeatedly perceives threat or uncertainty, the HPA axis remains engaged. Elevated stress activation can influence sleep, digestion, immune signalling, and hormonal balance.
This is not about blame.
It is about biology.
Protection Mode is adaptive.
But it is not the same as Creation Mode.

From Collapse to Recovery
At 35, I was doing everything “right.”
Following protocols.
Researching obsessively.
Trying to control every variable.
From the outside, I looked capable.
Inside, I was depleted.
I realised that while I was managing the strategy, I had never addressed the state.
My recovery did not begin with a new supplement.
It began when I stopped supervising my body and started rebuilding trust with it.
Less data.
More steadiness.
Less urgency.
More safety.
By the time I entered IVF at 39, my internal environment had shifted.
Not from control.
From regulation.
Why Most Clinics Prepare the Body, Not the Environment
Fertility clinics are exceptional at medical preparation.
They optimise follicles.
Time medication precisely.
Track hormone levels with extraordinary skill.
But emotional readiness is rarely measured.
And yet chronic stress activation can influence reproductive hormones, immune function, and treatment engagement.
When patients do not feel psychologically safe:
They underreport distress.
They disengage quietly.
They withdraw when cycles fail.
Emotional readiness is not a “nice extra.”
It is infrastructure.
Moving From Protection to Creation
Emotional readiness is the shift from managing your body to partnering with it.
From vigilance to regulation.
From urgency to steadiness.
Creation Mode does not remove uncertainty.
It increases your capacity to hold it.
Before your next cycle, ask yourself:
Am I moving forward from pressure —
or from steadiness?
A Gentle Next Step
If you are preparing for IVF in the next few months and want clarity about where your emotional readiness stands, I created a 7-minute IVF Emotional Readiness Scorecard.
It measures ten domains of preparation and highlights whether your system is operating in Protection Mode or Creation Mode.
You do not need to be fearless.
You only need to feel safe enough to begin.
Take the Scorecard here:
👉 https://form.typeform.com/to/LMWq32X0